REQUEST AN APPOINTMENT OR BOOK A CONSULANT – Sargam.dange.18@gmail.com
Osteoarthritis (OA) is the most common degenerative joint disorder and a major public health problem throughout the world. It affects any joint containing hyaline cartilage and the knees are the most commonly affected joints. Prevalence of OA increases with age and aging is associated with decreasing physiological functions, thus leading to major health problems. As a larger proportion of the elderly population in developed countries increasingly lives to an extreme old age, OA will be more prevalent and will be an important cause of disability in the future.
Although osteoarthritis can damage any joint, the disorder most commonly affects joints in your hands, knees, hips and spine.
Osteoarthritis symptoms can usually be managed, although the damage to joints can’t be reversed. Staying active, maintaining a healthy weight and some treatments might slow progression of the disease and help improve pain and joint function.
Symptoms
Osteoarthritis symptoms often develop slowly and worsen over time. Signs and symptoms of osteoarthritis include:
- Pain. Affected joints might hurt during or after movement.
- Stiffness. Joint stiffness might be most noticeable upon awakening or after being inactive.
- Tenderness. Your joint might feel tender when you apply light pressure to or near it.
- Loss of flexibility. You might not be able to move your joint through its full range of motion.
- Grating sensation. You might feel a grating sensation when you use the joint, and you might hear popping or crackling.
- Bone spurs. These extra bits of bone, which feel like hard lumps, can form around the affected joint.
- Swelling. This might be caused by soft tissue inflammation around the joint.
Osteoarthritis commonly affects the hands, feet, spine, and the large weight-bearing joints, such as the hips and knees, although in theory, any joint in the body can be affected. As osteoarthritis progresses, movement patterns (such as gait), are typically affected.Osteoarthritis is the most common cause of a joint effusion of the knee.
In smaller joints, such as at the fingers, hard bony enlargements, called Heberden’s nodes (on the distal interphalangeal joints) or Bouchard’s nodes (on the proximal interphalangeal joints), may form, and though they are not necessarily painful, they do limit the movement of the fingers significantly. Osteoarthritis of the toes may be a factor causing formation of bunions,rendering them red or swollen.

causes–
Damage from mechanical stress with insufficient self repair by joints is believed to be the primary cause of osteoarthritis. Sources of this stress may include misalignments of bones caused by congenital or pathogenic causes; mechanical injury; excess body weight; loss of strength in the muscles supporting a joint; and impairment of peripheral nerves, leading to sudden or uncoordinated movements. However exercise, including running in the absence of injury, has not been found to increase the risk of knee osteoarthritis. Nor has cracking one’s knuckles been found to play a role.
REQUEST AN APPOINTMENT OR BOOK A CONSULANT – Sargam.dange.18@gmail.com
Primary
The development of osteoarthritis is correlated with a history of previous joint injury and with obesity, especially with respect to knees. Changes in sex hormone levels may play a role in the development of osteoarthritis, as it is more prevalent among post-menopausal women than among men of the same age.Conflicting evidence exists for the differences in hip and knee osteoarthritis in African American and Caucasians.
Occupational
See also: Occupational disease and Occupational injury
Increased risk of developing knee and hip osteoarthritis was found among those who work with manual handling (e.g. lifting), have physically demanding work, walk at work, and have climbing tasks at work (e.g. climb stairs or ladders). With hip osteoarthritis in particular, increased risk of development over time was found among those who work in bent or twisted positions. For knee osteoarthritis in particular, increased risk was found among those who work in a kneeling or squatting position, experience heavy lifting in combination with a kneeling or squatting posture, and work standing up. Women and men have similar occupational risks for the development of osteoarthritis.
Secondary
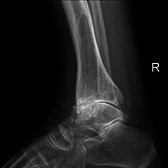
Lateral

FrontalSecondary osteoarthritis of the ankle (due to an old bone fracture) in an 82-year-old woman
This type of osteoarthritis is caused by other factors but the resulting pathology is the same as for primary osteoarthritis:
- Alkaptonuria
- Congenital disorders of joints
- Diabetes doubles the risk of having a joint replacement due to osteoarthritis and people with diabetes have joint replacements at a younger age than those without diabetes.
- Ehlers-Danlos syndrome
- Hemochromatosis and Wilson’s disease
- Inflammatory diseases (such as Perthes’ disease), (Lyme disease), and all chronic forms of arthritis (e.g., costochondritis, gout, and rheumatoid arthritis). In gout, uric acid crystals cause the cartilage to degenerate at a faster pace.
- Injury to joints or ligaments (such as the ACL), as a result of an accident or orthopedic operations.
- Ligamentous deterioration or instability may be a factor.
- Marfan syndrome
- Obesity
- Joint infection
REQUEST AN APPOINTMENT OR BOOK A CONSULANT – Sargam.dange.18@gmail.com
Risk factors
Factors that can increase your risk of osteoarthritis include:
- Older age. The risk of osteoarthritis increases with age.
- Sex. Women are more likely to develop osteoarthritis, though it isn’t clear why.
- Obesity. Carrying extra body weight contributes to osteoarthritis in several ways, and the more you weigh, the greater your risk. Increased weight adds stress to weight-bearing joints, such as your hips and knees. Also, fat tissue produces proteins that can cause harmful inflammation in and around your joints.
- Joint injuries. Injuries, such as those that occur when playing sports or from an accident, can increase the risk of osteoarthritis. Even injuries that occurred many years ago and seemingly healed can increase your risk of osteoarthritis.
- Repeated stress on the joint. If your job or a sport you play places repetitive stress on a joint, that joint might eventually develop osteoarthritis.
- Genetics. Some people inherit a tendency to develop osteoarthritis.
- Bone deformities. Some people are born with malformed joints or defective cartilage.
- Certain metabolic diseases. These include diabetes and a condition in which your body has too much iron (hemochromatosis
treatment–physiotherapy
Physiotherapy can involve a number of different treatment and preventative approaches, depending on the specific problems you’re experiencing.
At your first appointment, you will have an assessment to help determine what help you might need.
Three of the main approaches a physiotherapist may use are:
- education and advice
- movement and exercise
- manual therapy
Sometimes other techniques, such as acupuncture or ultrasound treatment, may also be tried.
Education and advice
One of the main aspects of physiotherapy involves looking at the body as a whole, rather than focusing on the individual factors of an injury.
Therefore, giving general advice about ways to improve your wellbeing – for example, by taking regular exercise and maintaining a healthy weight for your height and build – is an important part of treatment.
A physiotherapist can also give you specific advice that you can apply to everyday activities to look after yourself and reduce your risk of pain or injury.
For example, if you have back pain, you may be given advice about good posture, correct lifting or carrying techniques, and avoiding awkward twisting, over-stretching or prolonged standing.
Movement and exercise
Physiotherapists usually recommend movement and exercise to help improve your mobility and function. This may include:
- exercises designed to improve movement and strength in a specific part of the body – these usually need to be repeated regularly for a set length of time
- activities that involve moving your whole body, such as walking or swimming – these can help if you’re recovering from an operation or injury that affects your mobility
- exercises carried out in warm, shallow water (hydrotherapy or aquatic therapy) – the water can help relax and support the muscles and joints, while providing resistance to help you gradually get stronger
- advice and exercises to help you increase or maintain your physical activity – advice will be given on the importance of keeping active, and how to do this in a safe, effective way
- providing mobility aids – such as crutches or a walking stick to help you move around
Your physiotherapist may also recommend exercises that you can continue doing to help you manage pain in the long term or reduce your risk of injuring yourself again.
You can find exercise advice leaflets for some common problems, as well as exercises to prevent falls, on the Chartered Society of Physiotherapy (CSP) website.
REQUEST AN APPOINTMENT OR BOOK A CONSULANT – Sargam.dange.18@gmail.com
Manual therapy
Manual therapy is a technique where a physiotherapist uses their hands to manipulate, mobilise and massage the body tissues.
This can help:
- relieve pain and stiffness
- improve blood circulation
- help fluid drain more efficiently from parts of the body
- improve the movement of different parts of the body
- promote relaxation
Manual therapy can be used to treat specific problems, such as back pain, but may also be useful for a range of conditions that don’t affect the bones, joints or muscles.
For example, massage may improve quality of life for some people with serious or long-term conditions by reducing levels of anxiety and improving sleep quality. Manual techniques are also used to help certain lung conditions.
Other techniques
Other techniques sometimes used by physiotherapists that may help to ease pain and promote healing include:
- acupuncture – where fine needles are inserted into specific points of the body, with the aim of reducing pain and promoting recovery
- transcutaneous electrical nerve stimulation (TENS) – a small, battery-operated device is used to deliver an electric current to the affected area, with the aim of relieving pain
- ultrasound – where high-frequency sound waves are used to treat deep tissue injuries by stimulating blood circulation and cell activity, with the aim of reducing pain and spasms, as well as speeding up healing

REQUEST AN APPOINTMENT OR BOOK A CONSULANT – Sargam.dange.18@gmail.com
Thanks so much for giving everyone an exceptionally breathtaking possiblity to check tips from this site. It is always very ideal and also stuffed with a good time for me and my office acquaintances to visit the blog particularly thrice a week to read the fresh issues you will have. And definitely, I am just always fulfilled with the brilliant solutions you give. Selected two tips on this page are definitely the most beneficial I have ever had.
LikeLiked by 1 person